Click a topic to learn more about:
- Irregular periods
- Cysts and PCOS
- Endometriosis
- PMS / PMDD / Depression
- Postpartum depression
- Hormone imbalance
Natural treatments for reproductive and menstrual disorders
If you’re having trouble with irregular periods and other reproductive or menstrual disorders, you’re not alone. Symptoms may include cramps, irregular cycles, irregular and/or painful periods, recurring ovarian cysts, and more. Generally, most medical providers prescribe hormonal birth control or other contraceptives in response to these period problems. These drugs use synthetic hormones to override the natural cycle, masking the hormonal imbalance that may be the source of these symptoms. Birth control can also cause side effects and may even seriously harm some women.
Most medical providers aren’t aware that there are better options for treating, rather than masking, the causes of irregular periods or other menstrual disorders. Fertility awareness methods (FAM) are science-backed methods that equip women to effectively chart her fertility cycles, providing a wealth of information about an individual woman’s reproductive health. This information can assist FAM-trained doctors to tell what is really going on with your individual cycle, diagnose any issues, and design the treatment for your reproductive or menstrual disorder accordingly.
The fertility awareness approach to women’s health and fertility identifies any problems with a woman’s cycle by utilizing her fertility charts and other diagnostic tests and technologies, and then using this information to prescribe her a precise, individualized treatment for her menstrual disorder. Doctors who know how to use FAM charts to assist their patients in diagnosis and treatment of menstrual disorders are specialists in what is called Restorative Reproductive Medicine (RRM).
While doctors trained in RRM are growing in number, most mainstream doctors are uninformed about these technologies. Still, patients can seek and find doctors trained in RRM for telehealth or consulting regarding their menstrual or reproductive disorders. Professional institutions and organizations promoting and practicing RRM have opened a new path of diagnosis and treatment for many common reproductive disorders. NaProTechnology, in particular, has been helping women with irregular periods and other menstrual and reproductive disorders for decades. Developed over the last 30 years by Dr. Thomas Hilgers, NaProTechnology is supported by extensive peer-reviewed research data.
Irregular periods
What exactly is an “irregular period?” The actual definition of an irregular period is when a woman experiences one of the following conditions on a consistent basis: a) her period is shorter than 21 days or longer than 36 days; or b) her period varies by 5 or more days (e.g., one cycle is 22 days long, then the next is 40 days long, and the next is 34 days long, and so on.)
Irregular periods can be normal at certain points in a woman’s fertility, especially during the transitional phases of fertility, e.g., the onset of puberty, during breastfeeding, and during perimenopause. But if a woman is not in a transitional stage of fertility, and consistently experiencing irregular periods, they may be a symptom of an underlying reproductive disorder.
While young women are often prescribed hormonal birth control to “regulate” their periods, hormonal contraceptives do not actually regulate periods: birth control instead uses synthetic hormones to override a woman’s cycle, keeping her from ovulating and menstruating. The monthly bleeding experienced by a woman on birth control is not actually a period, but a withdrawal bleed.
Contrary to popular belief, it is possible to chart your menstrual cycle, even if you have irregular periods! In fact, charting your cycle with a fertility awareness method (FAM) can help you and an RRM-trained doctor get to the root of your irregular period symptoms, without using birth control.
For more information and resources on irregular periods, click here.
Ovarian cysts and Polycystic Ovary Syndrome (PCOS)
Some cyclic, one-sided pelvic and lower abdominal pain can be attributed to mittelschmerz, otherwise known as ovulation pain. But chronic pelvic pain on one or both side of your lower abdomen and pelvis can be an indication of ovarian cysts.
Different types of ovarian cysts exit, and some are more serious than others. Knowing the type of ovarian cysts you have and the cause of those cysts is an important part of getting the right kind of treatment for them.
A physician trained in Restorative Reproductive Medicine can use your fertility cycle charts and other diagnostic tests (such as blood tests and ultrasounds) to determine whether you have the condition known as polycystic ovary syndrome (PCOS). With this information, they can prescribe lifestyle changes and treatments (such as supplementation with bioidentical hormones) that may help treat the root cause of your PCOS symptoms. In some cases, surgical treatment for ovarian cysts may be necessary.
For more information and resources on ovarian cysts and PCOS, click here.
Endometriosis
Endometriosis is a disorder where tissue similar to that which lines the uterus (called the endometrium) grows outside of the uterus. The most common symptom of endometriosis is pain. This pain typically occurs in the lower abdominal area and lower back, but it can also occur in the hips and legs, or even (rarely) the chest.
Endometriosis is not well understood, and for a variety of reasons (including lack of patient and provider awareness, dismissal of women’s pain, and misdiagnosis) can take an average of 8 years to diagnose from the onset of symptoms.
Learning to chart your cycle with the help of a trained Fertility Awareness Method instructor and/or a medical provider familiar with your Fertility Awareness Method can help you detect signs of endometriosis. Doctors trained in Restorative Reproductive Medicine have pioneered various surgical techniques for the treatment of endometriosis in an attempt to manage the disease itself (rather than just its symptoms). Treatment may involve laparoscopic surgery to excise the lesions caused by endometriosis, as well as diet, exercise, and nutritional supplementation.
For more information and resources on endometriosis, click here.
Premenstrual Syndrome (PMS) / Premenstrual Dysphoric Disorder (PMDD) / Depression
PMS
If you’re a woman of reproductive age, chances are that at some point you’ve experienced an uncomfortable combination of symptoms warning you about your period’s arrival—symptoms like headaches, mood swings, irritability, or bloating before your period, and more. There isn’t a unified consensus about what exactly causes this phenomenon, often referred to as premenstrual syndrome (PMS). Some PMS symptoms are likely a normal sign of the hormonal shifts that naturally occur during a woman’s cycle.
Some girls and women may be more sensitive to these natural hormonal fluctuations than others. They may experience more severe symptoms of PMS, which may cause them to miss school or work. Some researchers theorize that a hormonal imbalance (namely low progesterone) may be at play with more severe PMS symptoms. Various dietary and lifestyle choices may also contribute to certain PMS symptoms, including overconsumption of sugar, lack of sleep, and stress. Doctors trained in Restorative Reproductive Medicine can assist women in treating PMS without requiring them to take synthetic hormones or birth control.
PMDD
Premenstrual Dysphoric Disorder or PMDD is a unique, and debilitating health condition. A woman with PMDD experiences extreme depression, irritability, anxiety, or anger in the two weeks leading up to her period. PMDD is far more severe than the moodiness and general irritability that many women often experience as part of PMS. Women with PMDD cannot function in everyday life, and may be at risk of harming themselves or others.
Researchers are uncertain as to why PMDD occurs in some women but not others. There are a few theories that may explain why PMS escalates to PMDD, ranging from a progesterone deficiency, to diminished serotonin activity triggered by the ovarian cycle. Doctors trained in Restorative Reproductive Medicine can help women suffering with PMDD to find effective treatments to restore their hormonal balance.
Depression
Some women may mistake PMS moodiness or the periodic, extreme mood swings of PMDD for an underlying, generalized depression or anxiety disorder, conditions which often worsen in the days leading up to one’s period. If your anxious or depressive symptoms do not completely resolve when your period begins, you may actually have a depression or anxiety disorder. Charting your cycle can help you keep better track of when your anxious or depressive symptoms begin and end, and how they correlate with changes in your cycle.
While doctors are often quick to prescribe birth control to combat PMS and PMDD, researchers have recently uncovered a significant link between birth control use and depression, especially among young women. Thankfully, doctors trained in Restorative Reproductive Medicine techniques have the ability to treat PMS and PMDD without the use of the synthetic hormones found in birth control, which may make depression worse.
For more information and resources on PMS, PMDD, and depression, click here.
For more information and resources on birth control and depression, click here.
Postpartum Depression (PPD)
Women may be especially at risk for developing depression during the postpartum time.
Like general depression, postpartum depression (PPD) is a serious mental health issue requiring medical attention. While approximately 70% of women experience “the baby blues” after giving birth, the feelings of sadness and anxiety associated with the baby blues typically only last for a few days postpartum. The symptoms of PPD are more severe and last for two or more weeks.
Some women may require antidepressant medication and/or psychotherapy to treat their PPD. Doctors trained in restorative reproductive medicine may be able to treat PPD with hormone therapy.
For more information and resources on postpartum depression, click here.
Hormone imbalance
Hormone imbalances can make themselves apparent through a variety of symptoms including painful and heavy periods, pelvic or lower abdominal cramps, cystic acne, low sex drive, moodiness, and more. Hormonal imbalances can also make conceiving and carrying a pregnancy to term difficult.
It’s important to learn about the root causes of hormonal imbalances so you can pursue effective treatments, instead of simply covering up the symptoms with drugs like hormonal birth control. Doctors trained in Restorative Reproductive Medicine can assist patients with hormonal imbalances by restoring their natural hormone levels with tailored treatments of bioidentical hormones to support her natural cycle, as opposed to synthetic hormones (such as those found in hormonal contraceptives) that override one’s natural cycle.
For more information and resources on hormonal imbalances, click here.
If you believe you could be suffering from one or more of the reproductive or menstrual disorders described above, know that help is available. Learning to chart your cycles with a Fertility Awareness Method can be a great first step towards helping your doctor identify the root causes of your reproductive or menstrual disorder, so that you can get authentic treatment, tailored to your unique needs.
-

How Fertility Awareness Can Help with Severe Menstrual Cramps
By Katherine Young • February 13, 2021Dysmenorrhea, or severe menstrual cramps, is a common and debilitating issue for many women. Fertility Awareness Methods (FAM) can… -

8 non-pharmaceutical options for pregnancy pain relief
By Kaitlyn Kulda • February 25, 2025Pregnancy can sometimes feel like a tightrope between very high-stakes “do’s” and “don’ts.” Do drink raspberry leaf tea… -

What’s the connection between endometriosis and ovarian cancer?
By Caitlin Estes • January 4, 2025A 2024 study published in the Journal of the American Medical Association (JAMA) found that women with endometriosis… -

Heavy periods and heart disease: What’s the connection?
By Melayna Alicea • December 12, 2024The link between heavy menstrual bleeding and cardiovascular disease -

Natural Womanhood Book Review: Period Repair Manual
By Kaitlyn Kulda • October 26, 2024Our full review and rec on whether to buy, borrow, or pass -

Could cabergoline be a new treatment for endometriosis?
By Elizabeth Wescott, PhD • October 3, 2024What we know so far -

In praise of Magnesium: What this essential mineral does for the body
By Jaclyn Brown • September 5, 2024And it’s connection to fertility -

What this popular health website got right (and wrong) about natural birth control
By Caitlin Estes • August 22, 2024Can we please stop telling women with irregular periods they can’t use FAM? -

What is progesterone resistance?
By Caitlin Estes • April 20, 2024And the role it may play in miscarriage and endometriosis -
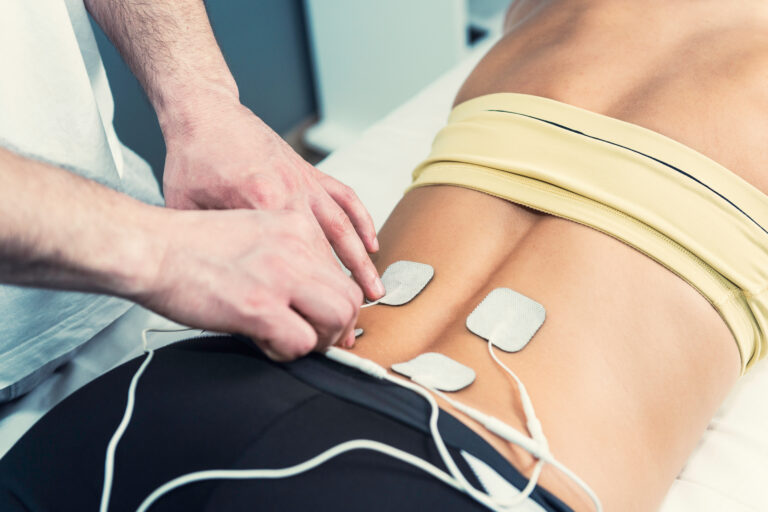
Can a TENS unit help with period or endometriosis pain?
By Melayna Alicea • March 28, 2024How to customize settings for max pain relief




