Endometriosis affects approximately 89 million women worldwide. It affects all ages and races, and is one of the leading causes of female infertility.
Pain from endometriosis (often referred to as simply “endo”) causes girls and women to miss school and work—or perhaps worse—to endure both while in excruciating pain. For as common as it is, very little is known about this disorder.
What is endometriosis?
Endometriosis is a disorder where tissue similar to that which lines the uterus (called the endometrium) grows outside of the uterus. This tissue typically grows on other organs in the pelvic area, such as the ovaries and fallopian tubes. Just like the endometrium, this tissue also breaks down and bleeds during menstruation, but because it has no way to exit the body, it stays in the pelvic area. The trapped blood and tissue eventually forms scar tissue and adhesions, bands of tissue that grow between pelvic organs and cause them to stick together.
What are the symptoms of endometriosis?
The most common symptom of endo is pain. Endometriosis is associated with especially severe pain during periods that is much worse than typical menstrual cramps. Pain with sex is also reported. Oddly enough, the level of pain someone experiences is not a good gauge of how advanced the disease is. Some women may have very little scarring, and an inordinate amount of pain; others may have very extensive scarring, yet little to no pain. Laparoscopic surgery is necessary to make a formal diagnosis.
What causes endometriosis?
Endometriosis is not well understood, and for a variety of reasons (including lack of patient and provider awareness, dismissal of women’s pain, and misdiagnosis) takes an average of 8 years to diagnose from the onset of symptoms. The exact cause of the disease is also unknown, although multiple theories abound. Some research suggests a connection between endo and autoimmune diseases but further investigation is needed to confirm the nature of the relationship. Estrogen dominance may also contribute to this disease and to other reproductive disorders. Perhaps one of the reasons we know so little about endometriosis is because young women are often placed on symptom-masking hormonal birth control as soon as they present with menstrual difficulty, only to come off of it later in life (perhaps when they wish to get pregnant), and find that the disorder neve really went away while they were on the pill.
Can I use a fertility awareness method with endometriosis?
Yes! In fact, learning to chart your cycle with the help of a trained instructor and/or a medical provider familiar with your FABM can help you detect signs of endometriosis.
Is endometriosis treatable?
Hormonal contraception is often prescribed to manage the symptoms of this disorder, but it cannot cure it. In fact, birth control could make endo worse. Natural Procreative Technology physicians (also known as NaPro doctors) have pioneered various surgical techniques for the treatment of endo in an attempt to manage the disease itself (rather than just its symptoms). Treatment may involve laparoscopic surgery to excise the lesions caused by endometriosis, as well as diet, exercise, and nutritional supplementation. NaPro physicians are especially trained to perform this kind of surgery and offer other supportive care.
Is there a cure for endometriosis?
No, there is currently no cure for endo. Treatment for endometriosis does exist, however, and an anti-inflammatory diet and exercise to restore proper hormone balance may help naturally decrease endometriosis pain. For a long time, it was believed that pregnancy could “cure” endo, which we now know is a myth (although pregnancy may temporarily reduce symptoms). Actress Lena Dunham made headlines with her decision to have a hysterectomy to cure her endometriosis, but the Endometriosis Association warns that “combined with thorough excision, [a hysterectomy] may reduce or eliminate symptoms; not a sure cure.”
Can endometriosis cause infertility?
Endometriosis is one of the leading causes of infertility. However, that does not mean that every woman with endo will be unable to conceive. If you are having trouble trying to conceive, it may be worth investigating whether or not you have endo or some other reproductive disorder. NaProTechnology physicians are especially trained to diagnose and treat endometriosis, which, if successful, may also cure a woman’s infertility.
For more on endometriosis, see the articles below.
-
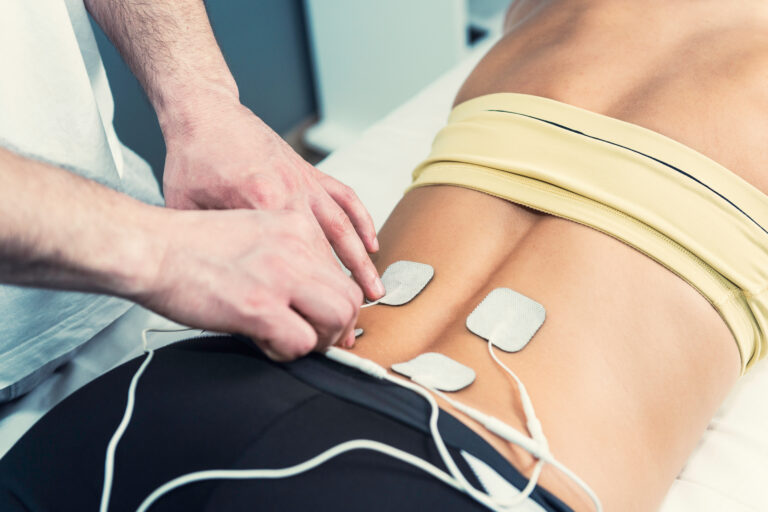
Can a TENS unit help with period or endometriosis pain?
By Melayna Alicea • March 28, 2024How to customize settings for max pain relief -

Celebrities with endometriosis: What we wish they knew
By Melayna Alicea • March 28, 2024Here’s what we’d tell Halsey, Lena Dunham, and Amy Schumer -

Diagnosing and treating endometriosis in the teen years
By Grace Emily Stark • March 27, 2024Getting young women help for Endo earlier with more aggressive treatment -

Endometriosis is usually diagnosed in adulthood. Does it appear during the teen years?
By Taryn DeLong • July 28, 2023“We shouldn’t be normalizing pain.” So says Dr. Jessica Shim, a pediatric and reproductive gynecologist and endometriosis specialist… -

“Sex should never be painful:” The connection between endometriosis and painful sex
By Mary Bruno • November 4, 2022Decked out in my white strapless dress trimmed with a subtle sweetheart neckline (and just a touch of… -

Three facts about endometriosis that prove it’s more than just a painful period disease
By Morganne Skinner, BSN, RN • September 16, 2022When you think of endometriosis, what comes to mind? You may already know that endometriosis can cause painful… -

8 ways endometriosis can make it more difficult to get pregnant
By Morganne Skinner, BSN, RN • August 18, 2022If you suffer from endometriosis, you are likely aware that it may have negative implications for your fertility.… -

Can acupuncture relieve your endometriosis-related period pain?
By Morganne Skinner, BSN, RN • June 17, 2022I remember sitting in my acupuncturist’s office seeking help for period pain when she asked, “And did you… -

Adenomyosis vs. Endometriosis: How they’re similar, and how they differ
By Anne Marie Williams, RN, BSN • February 24, 2022If you’ve ever gone to your general practitioner or OB/GYN with heavy bleeding, pain during sex, or spotting…





