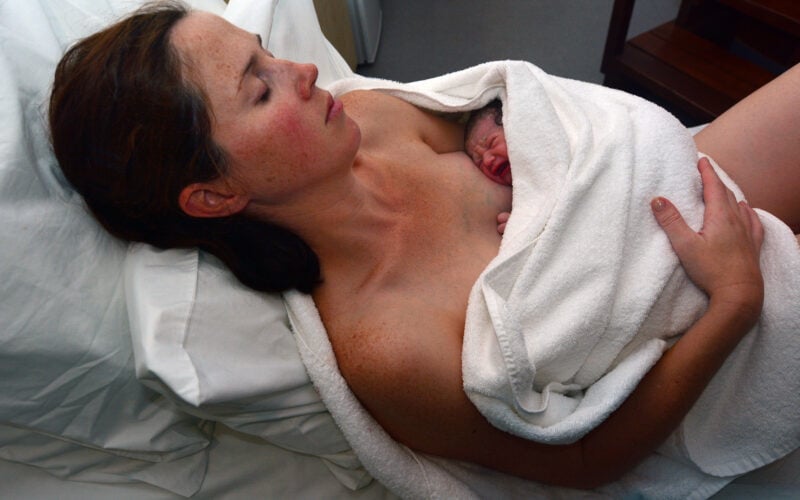
When I was pregnant with my first child, a “natural childbirth” was something only a select few of my “crunchy” friends chose. Colloquially defined as foregoing an epidural or other forms of anesthesia or pain medication during the labor process, a natural childbirth seemed unthinkable to me then, and I went into labor planning on having an epidural. This was the twenty-first century; of course I was going to take advantage of the benefits of modern medicine.
My thinking has shifted substantially in the years since, instigated in part by my own far-from-ideal epidural experience. And while I have no intention of throwing shade on women who want epidurals (many of whom have positive experiences!) or need anesthesia as part of a Cesarean birth, looking back, my own automatic dismissal of “natural childbirth” reflected a lack of understanding about the good and beautiful design of women’s bodies. Since that first birth, I have gone on to have two successful, epidural-free births. Here are the six things I think every woman considering a natural childbirth needs to know.
#1 You were made to do this
Our societal acceptance of the alteration, suppression, or destruction of our fertility through contraception has regrettably bled over into our approach to pregnancy, labor, and childbirth. That’s one of the eye-opening connections made by author Leah Jacobson in her new book, Wholistic Feminism. Once we’ve accepted the premise that our bodies are broken and in need of manipulation or control via contraception, Jacobson argues, we’re less likely to believe our bodies were in fact, to use the words of a birthing class taught by a popular California doula and YouTuber, “built to birth.”
In contrast to the false “women’s bodies are broken” paradigm, Jacobson advocates embracing women’s uniquely feminine capabilities to “ovulate, gestate, and lactate.” Jacobson notes that it is “the tendency of modern medicine to ‘take over’ [the birth process]… supposedly for the ease and convenience of the laboring mother.” However, this can leave a birthing mother feeling anxious, overwhelmed, and out of control during the labor and delivery process. In contrast, Jacobson points out that “for women who understand how to surrender and how to trust in the design of their bodies, pregnancy and childbirth can be incredibly spiritual and an empowering experience.” (Jacobson, 53-54)
“Empowering” is definitely a word I would choose to describe my second birth. A 32-year veteran labor and delivery nurse coached me by teaching me what to expect, and guided me through various position changes to facilitate the baby’s cardinal movements (i.e., the movements the baby’s head goes through, starting just before labor and continuing all the way through the time of birth). Unhindered by the numbing effects of an epidural, I was able to utilize the pain as a natural guide to assume the positions that would most help my baby descend and flex, internally rotate, extend, externally rotate, and then come out!
#2 Dilation is only one part of the picture
Labor and delivery nurse and certified childbirth educator Elizabeth, creator of the popular “Nurse Zabe” YouTube channel, notes that cervical dilation is only part of the picture of how a woman is progressing in labor, meaning that that number, i.e. “you’re 4 centimeters dilated” or “you’re 8 centimeters dilated” really is just a number, and not necessarily indicative of how far away your baby’s birth is. As Natural Womanhood’s Editor, Grace Emily Stark, relates:
“During my last childbirth, my midwife did not want me to get discouraged about how long the last few centimeters of dilation were taking me to achieve. She said ‘I’ve seen women where you’re at have a baby in their arms 20 minutes later!’”
Besides dilation, another key component is the baby’s location in relation to mom’s pelvis. During labor, baby’s head will drop into the pelvic inlet, then descend through the mid-pelvis, then the pelvic outlet, and finally through the birth canal on the way to greet the outside world. Given that a baby will always take the path of least resistance on the way down and out, maternal position changes can physically facilitate the birthing process.
#3 Movement is magical
Nurse Zabe offers an incredibly informative explanation on the importance of movement and repositioning in labor for both mom and baby.
“The really cool thing about movement in labor is that you’ll notice it’s almost instinctual. If you are not fighting your contractions, if you’re kind of allowing them to happen, not only do these movements help move baby, help dilate your cervix, they also help create a rhythm and a ritual to your labor to help you cope with your contractions.”
Showering, walking around (whether in your house or around the hospital room or through the hospital hallways), utilizing a birthing ball, squatting, and more can all be very helpful.
Specific positions may help facilitate baby’s movement through the pelvic inlet, mid pelvis, and pelvic outlet. Positions with wide knees and feet together (as in a deep squat or lying on the bed with a peanut-shaped birthing ball between the knees) help baby descend through the inlet. Knees closer together and asymmetrical movements (like lying in bed with one knee up towards the chin, or standing with one leg up on the bed) facilitate baby’s movement through the mid-pelvis. Finally, having your knees closer together and feet further apart (as in side-lying position on the bed with a peanut birthing ball between the feet) can help open up the outlet.
As Nurse Zabe stresses, if you’re open to the process and listen to your body, you’ll typically find that you instinctually move in certain ways. You may rock backwards and forward to guide baby into the inlet, and side to side to wiggle baby through the narrowest part of the pelvis (the mid-pelvis). You may stand up on tip-toe on one leg to help baby through the pelvic outlet.
She emphasizes, “Movement is magical! Movement is key!”
#4 Pushing feels… familiar
I’ll never forget the example that the veteran L&D nurse gave me to explain how I’d know when it was time to push. She told me that as I got close, I would feel rectal pressure, “like when you’re at the mall and you have to poop, but you don’t want to go in a public restroom so you hold it til you get home.” When it was time to push, though, she said, it’d be “like being at the mall, but you don’t care where you are. You have to go NOW!”
Truth be told, that’s exactly how I felt when it was time to push.
Whereas with my first child I had pushed clumsily, with coaching, and without really having any idea how to do so because I couldn’t feel anything, the second time around I suddenly felt that my body was spontaneously starting to push. I had no control over it. The same thing happened with my third birth–I couldn’t have stopped the pushing if I’d wanted to. My body just took over.
And, by the way, a really good midwife, experienced labor and delivery nurse, or veteran OB/GYN doesn’t necessarily need to check how dilated you are to know when it’s time for you to push… they can tell by the sounds you’re making. Isn’t that amazing? As Grace Emily Stark relates:
“As I got toward the end of my last birth, I could hear myself starting to make even lower and louder sounds–but I was feeling nervous and second-guessing myself about whether it might be time to start pushing. That’s when my midwife walked in the room and said ‘Okay, it sounds like it’s time for you to start pushing!’ When I said ‘Really?! Are you sure??’ She said, ‘Well, you either sound like a woman about to have a baby, or you’re doing a very good impression of one!’”
#5 When you feel like you can’t do anymore, surrender
Surrender is key in the natural childbirth process. Being educated ahead of time on the distinct stages of labor (a brief overview is here), how you might feel during each one— especially during “transition,” when virtually every woman experiences a distinct feeling of “I can’t do this anymore!”—and your options for pain management, can help you surrender to and cooperate with the hard work that your body is doing, and even instinctively knows how to do with adequate support. Knowing what I’d feel like when pushing was about to start helped me to trust the process rather than resisting it, and to focus and buckle down because the end was in sight.
I also learned from the “mother of modern midwifery,” Ina May Gaskins, in her book Ina May’s Guide to Childbirth, that many women struggle to relax their pelvic floor during labor (as opposed to contracting it as one does during a Kegel). Ina May says that the tension or relaxation of the jaw is actually a direct indicator of the rigidity or relaxation of the pelvic floor. Therefore, if you loosen the jaw with breathing and open-mouthed, low-pitched sounds, you’ll relax the pelvic floor at the same time.
#6 You’re going to need support
Cassie Moriarty, a doula and lactation consultant, told Natural Womanhood:
“We forget that birth is driven by hormones which are driven by the environment in which the mom is in. The hormones experienced at birth are some of the same ones experienced during intercourse. Think about what is needed to feel safe, comfortable, secure, warm during intercourse. The same is true of birth. This is why a mom’s labor can slow when she walks through the hospital doors. The body can have trouble feeling safe, comfortable, secure in a crowded building with fluorescent lights, people coughing, long lines, and strange machines beeping.” Moriarty notes, “It’s not that women must be Herculean to make it through childbirth, but rather their support system and birthing location must support the wisdom of the birthing body.”
Assuming that vaginal delivery makes sense based on your medical history, you absolutely can have a natural childbirth… but you’re going to need help. Sure, you need to have a provider who supports you, but that’s not enough since they may not be with you throughout the whole labor and delivery process (especially if you’re delivering in a hospital). And since preparation is key (including physical preparation for labor), you’ll need to proactively identify who your support person or people will be.
Keep in mind that your support person, whether a friend, family member, or doula, should not just “show up” for the labor and delivery. This person should either learn along with you about unmedicated or low-intervention birth, or already have experience coaching or supporting moms through the natural childbirth process.
You’re not crazy for entertaining the idea of a natural childbirth—and you don’t need to be “crunchy granola” to do it—but it isn’t a walk in the park, and you’ll need to prepare. A good birthing class or book will go into even more detail on all the points I’ve enumerated above, and is an excellent investment in your—and your baby’s—future birthing experience.
Additional Reading:
Three science-backed, natural ways to ease childbirth and the postpartum period
Giving birth naturally, a beautiful option
The fourth trimester guidebook: postpartum nutrition
The fourth trimester guidebook: postpartum healing and exercise
The fourth trimester guidebook: your postpartum mental health matters