Jessica, who asked that her name be changed, suffered from menstrual migraines.
Jessica’s migraine always came at very inconvenient times—right before a busy day of dentist appointments for her children, during a date night with her husband, or in the middle of a trip to the park (really, though, is there EVER a convenient time to get a migraine?). For many years, migraines prevented Jessica from being really present to her husband and her four homeschooled children. The migraines were so debilitating that she was willing to try anything to feel better. It seemed hopeless—until Jessica noticed that her migraines came at the same time in her cycle each month.
Chances are, you or someone you know experiences migraines on a regular basis. According to the Migraine Research Foundation (MRF), 18 percent of American women have migraines (compared to 6 percent of men) and more than 90 percent of migraine sufferers miss work or can’t function normally during a migraine attack. MRF notes that “about half of female sufferers have more than one attack each month, and a quarter experience 4 or more severe attacks per month.” MRF also notes that “more severe and more frequent attacks often result from fluctuations in estrogen levels.” This, of course, gives rise to the suspicion that perhaps women’s hormones are at play in their increased susceptibility to migraines and headaches—hence the concept of menstrual migraines and hormonal headaches.
How do you know if it’s a headache or a migraine?
According to Penn Medicine, migraine is actually a neurological disease, which usually (although not always) includes head pain. The type of head pain involved in a migraine attack is usually characterized by severe, throbbing pain on one side of the head (although MRF notes that in about one-third of migraine attacks, both sides of the head are affected). The average range of time of a migraine attack is between 4 and 72 hours.
Unlike headaches, migraines are typically accompanied by one or more other disruptive symptoms, the most common of which are nausea, vomiting, visual disturbances (including aura), dizziness, and sensitivity to light and/or sound.
What is the connection between headaches, migraines, and hormones?
While Jessica experienced cycle-related migraines (known as menstrual migraines), hormonal headaches are common for women as well. In some cases, a hormonal headache or menstrual migraine episode is the direct result of an imbalance of hormones at certain times of the menstrual cycle. Unfortunately, menstrual migraine (i.e., a migraine that occurs between two days before to three days after your period begins) can be one of the most difficult types of migraines to treat—and also one of the most severely painful.
The late Dr. Seymour Diamond, author of The Hormone Headache and founder of the Chicago’s Diamond Headache Clinic, says, “headache activity increases…when estrogen levels are in flux, either rising or falling, or when there is a change in the estrogen-to-progesterone ratio.”
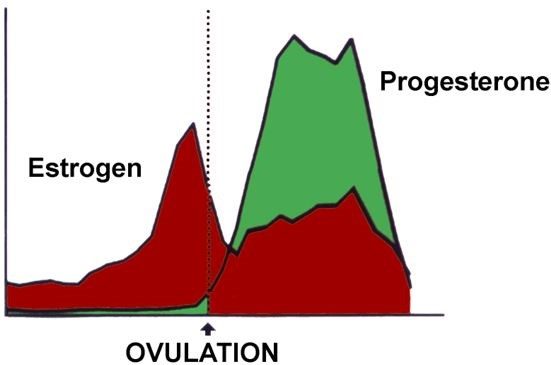
For women who are cycling (that is, pre-menopausal women who are not on hormonal birth control, which overrides the menstrual cycle), this fluctuation in estrogen levels happens immediately after ovulation and again with the start of menstruation. For a variety of reasons, it is problematic when a woman has unusually high levels of estrogen, and low levels of progesterone (often considered “estrogen dominance”). Estrogen dominance is common in women experiencing reproductive issues like polycystic ovary syndrome (PCOS) or endometriosis, and in teenagers who are just beginning to have menstrual cycles. Some women may also experience migraines and hormonal headaches in pregnancy and menopause, as these are also times of extreme hormonal fluctuation.
Will birth control help my hormonal headaches or menstrual migraines?
Because hormonal contraception overrides a woman’s natural menstrual cycle by providing a continuous dose of synthetic hormones, some women may begin birth control as a means of controlling headaches or migraines associated with the fluctuations of a natural menstrual cycle. However, migraine with aura is often a contraindication for the prescription of certain kinds of birth control (in layman’s terms, this means that if you have migraine with aura, your doctor should not prescribe you certain kinds of birth control, as it can increase your chance of stroke). And while some women with hormonal headaches or menstrual migraines may experience relief while on birth control, headaches and migraines are also among some of the most commonly reported side effects of hormonal birth control.
Preventing hormonal headaches or menstrual migraines
Instead of opting for birth control, a great place to start when experiencing recurrent headaches or migraines is to track your fertility for at least two cycles or two months, using what’s known in the medical community as a Fertility Awareness-Based Method, more informally called fertility awareness methods (FAM) or natural family planning (NFP). This step is critical: if the problem is related to a hormonal imbalance during your cycle, you need to identify at what stages of your cycle when the hormonal deficiency takes place. It is especially important to identify when you ovulate, which is different for every woman, and even from one cycle to another.
Restorative Reproductive Medicine (RRM) for hormonal headaches and/or menstrual migraines
If through charting you discover that your headaches or migraines are associated with fluctuations in your cycle, it is worth finding a medical provider who will dig more deeply into your hormones, rather than override them with the synthetic hormones found in birth control. You may have an underlying issue causing not only your headaches or migraines, but other reproductive issues as well.
A medical provider who takes your hormone-related headache or migraine concerns seriously, and who is trained to read your fertility charts, can order a hormonal panel of blood draws to get to the bottom of your hormonal headaches or menstrual migraines. The results of those draws will help your provider to prescribe bioidentical hormones (read: not synthetic!) to assist with balancing your hormones—and your cycle—if indicated. These kinds of hormones are often found at compounding pharmacies, which can be found throughout the U.S. and internationally. Bioidentical hormones actually mimic those made by our bodies (which is very different from the synthetic estrogen and progestin found in birth control products).
Beware the rebound headache: Consider natural remedies and lifestyle changes
A restorative reproductive medical provider can also discuss lifestyle considerations such as sleep, exercise, nutrition, and supplementation with you, in order to minimize or eliminate migraine or headache triggers.
Dr. Jolene Brighten, a naturopathic physician and author of Beyond the Pill, lists twenty different natural remedies and lifestyle changes for hormonal headaches, and notes that estrogen dominance is often a major culprit of cyclical, hormonal headaches and menstrual migraines. Again, tracking your fertility signs is an important way to help discover any potential hormonal imbalances, and it will also help you and your doctor pinpoint which supplements should be taken during specific parts of your cycle, in order to be the most effective. This is yet another way that a restorative reproductive medical provider will work with you to optimize your body’s natural functioning, rather than put a Band-Aid like birth control over the issue.
It’s also important to not overuse pain medication when dealing with cyclical or chronic headaches or migraines. While many of us are tempted to reach for medication when faced with a bad headache or migraine, overuse of medication can lead to what is known as rebound headaches. This can lead to a vicious cycle of one headache after another, as the medication used to relieve the pain of one headache can actually cause or trigger yet another headache or migraine. This is yet another excellent reason why getting to the root cause of your hormonal headaches or menstrual migraines can be invaluable for your overall health and wellbeing.
You don’t have to choose between pain and pregnancy
If you are considering getting off birth control to get to the root cause of your headaches or migraines, you may be concerned about the chance of getting pregnant. Fortunately, when you learn a fertility awareness method from a qualified instructor, these methods are as effective as common contraceptive methods when trying to avoid pregnancy. So, you absolutely do not have to give up effective family planning in the process of getting real treatment for your hormonal headaches or menstrual migraines!
In Jessica’s case, her physician developed a customized preventative and pro-active approach to treating her menstrual migraines. Jessica’s physician directed her to take naproxen (an anti-inflammatory) and bioidentical progesterone in the days after ovulation and supplement with magnesium during the time of ovulation. In addition, the doctor prescribed her a migraine medication to help the pain and symptoms subside if migraines did occur.
Thanks to her fertility awareness method, and a doctor who knew how to use the information found in Jessica’s charts, Jessica is no longer afflicted by frequent menstrual migraines. In fact, she rarely experiences them. Balancing her hormones through restorative therapies significantly decreased Jessica’s migraines and dramatically improved her quality of life. She no longer lives in constant worry about when and where she will get her next migraine.
When this article refers to fertility awareness methods (FAM), or natural family planning (NFP), we are referring to Fertility Awareness-Based Methods, evidence-based methods of cycle charting which can be used as effective forms of natural birth control when learned by a certified instructor.
This article was originally published on May 20, 2017 as written by Liz Escoffery. It has since been updated by Natural Womanhood to offer more resources. Last updated October 9, 2020.
Additional Reading:
Three Simple Tips to Limit Endocrine Disruptors and Balance Hormones Naturally
Progesterone Deficiency: How Too Little Progesterone Can Mean Big Problems







