We live during a time when the avantages pour la santé de l'allaitement for both mom and baby are well-established and relatively well-known, but taux of ever breastfeeding, or of breastfeeding exclusively at three or six months, or any amount at six months to one year remain low.
Why the discrepancy?
Particularly for moms who work outside the home and pump, or pump exclusively for other reasons, following the CDC’s guidelines for breast milk storage can lead to many tears over spilled (wasted) milk. In fact, a 2026 preprint study (not yet peer-reviewed) found that 46% of surveyed parents pitched leftover pumped milk quotidien [1].
Dans un deep dive for her popular ParentData website (behind a paywall but accessible with a 7-day free trial), Harvard-trained economist and bestselling author of Expecting Better, Cribsheet, The Family Firmet L'inattendu, Emily Oster argued that current guidelines are unnecessarily restrictive and could safely be loosened based on the available research. While the CDC recommendations are specifically intended to prevent bacterial growth in breastmilk, in a post on X, Oster labeled them “way too cautious.”
What the CDC guidelines on breastmilk storage say
The CDC has specific recommendations for freshly pumped vs. previously frozen breastmilk.
Parmi eux :
- Has the freshly pumped milk been out of the refrigerator for four hours? If so, pitch.
- Has the freshly pumped milk been in the refrigerator four days or longer? Toss.
- Has previously frozen, thawed breastmilk been out of the fridge for longer than deux hours? It’s gone.
- The same goes for thawed breastmilk that’s been in the fridge longer than 24 hours.
- What about a bottle the baby didn’t finish during a feeding (whether it was in the fridge or freshly pumped)? Pitch if older than two hours (yes, even though babies older than a few weeks are unlikely to take a bottle again so soon).
A mom following the CDC guidelines for breastmilk storage to a B (for breastmilk) will inevitably find herself between a rock and a hard place. Should she compromise her mental health trying to follow the guidelines, inevitably pitching large quantities of her hard-won, immune-boosting liquid gold in the process? Or should she disregard the guidelines and, so the thinking goes, potentially expose her baby to harm?
Not to worry, says Oster. There’s no need for moms to choose between their mental health and nourishing their babies with breastmilk.
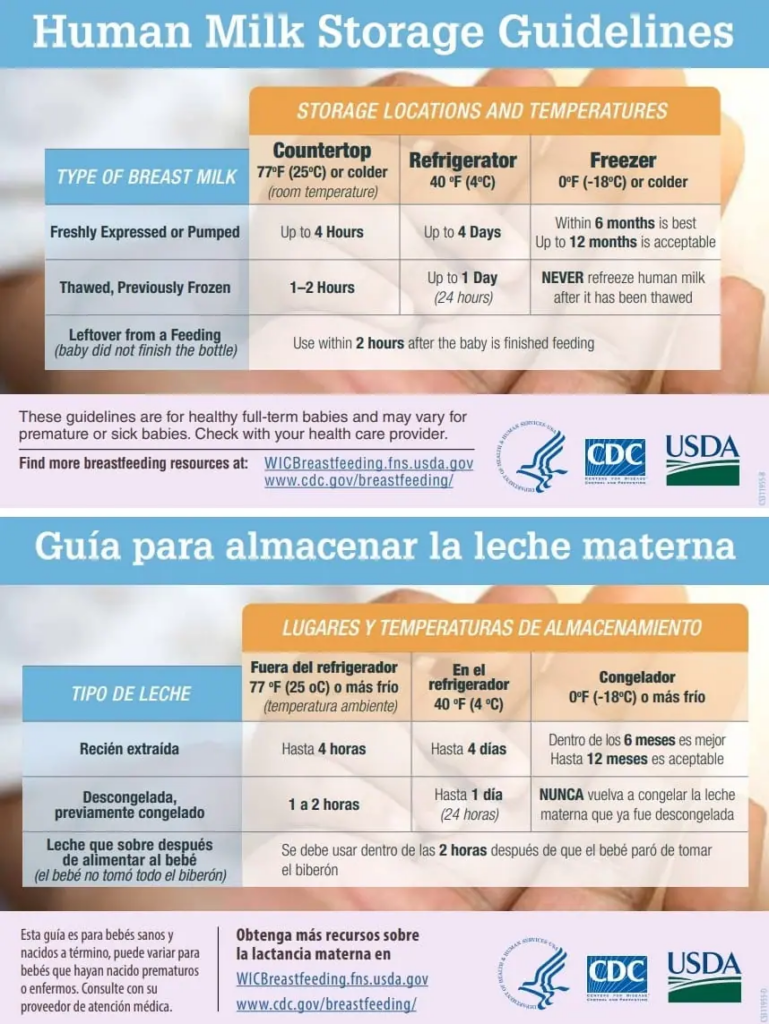
source: CDC.gov
Some bacteria in breastmilk is expected
Oster spelled out the facts when it comes to bacteria in breastmilk. First, there will always be some bacteria in even the freshest breastmilk. This is because the skin on the mother’s breast carries bacteria. Second, there will be additional bacteria from the baby’s mouth if a baby starts a bottle and finishes it at a second feeding. This is why the CDC warns against saving the rest for later. Third, bacteria multiply faster at hotter temperatures.
But, Oster observed, “It is important to note that [bacteria] levels matter here. There are bacteria everywhere and in everything, even some bad bacteria. At low levels, that’s OK. At high levels, however, you have to be careful, and there are guidelines about how high these bacterial levels can be before they cause a problem.”
We instinctively know that several days of sitting on the counter will spoil milk, and that an hour at room temp (generally considered 77 F) isn’t a problem. What does the data tell us about the in-between time? Oster broke down what we do and don’t yet know about safe breastmilk storage.
Breastmilk on the counter: How long is too long?
We’ve known for a full 30 years (thanks to this small 1996 study) that freshly pumped breastmilk is safe much longer than the CDC’s suggested four hours at room temperature [2]. In the study, milk kept on the counter in a 59 F room had no significant bacterial growth even 24 hours later. Growth remained low for up to 8 hours on the counter in a 77 F room. Even in a 100 F room, the milk had insignificant bacterial growth for 4 hours on the counter.
In the study, milk kept on the counter in a 59 F room had no significant bacterial growth even 24 hours later. Growth remained low for up to 8 hours on the counter in a 77 F room. Even in a 100 F room, the milk had insignificant bacterial growth for 4 hours on the counter.
A newer, also small 2013 study from Nigeria had comparable results [3]. Breastmilk had unconcerning bacterial growth for up to 9 hours in tropical conditions.
En outre, le 2026 preprint (not yet peer-reviewed) German study mentioned above found that breastmilk bacterial growth was unchanged over 24 hours at refrigerator temperature et at room temperature [1]. Oster’s takeaway? “This means if you accidentally leave pumped milk on the counter overnight, you may not need to throw it away.”
Breastmilk that’s been reheated can go back in the fridge, and you can mix cold and warm milk
Recall that the CDC frowns on keeping milk that’s been reheated and wasn’t used at all. The same goes for milk that’s been partially drunk and wasn’t finished within two hours. Similarly, freshly pumped, still-warm milk isn’t supposed to be added to a pitcher or bottle or storage bag of cold milk in the fridge. The concern in these cases, as always, is that warmed or warmer milk will lead to faster bacterial growth in the whole sample.
Referencing milk that’s been thawed and warmed mais was not drunk going back in the fridge, Oster weighs in, “Bacteria would grow slightly more quickly during the heated period and then slow down in the fridge. Overall, the storage timing would be similar to what it would be if you just had it in the fridge, maybe a bit shorter.”
When it comes to milk that was partially consumed, Oster connects the dots by first citing an old study finding that breastmilk is less susceptible to bacterial growth than formula, and putting that information together with the knowledge that partially drunk formula is safe up to 24 hours later [4] [5]. The preprint study comparably found that even 24 hours later, bacterial growth in partially drunk breastmilk was unconcerning [1].
When it comes to milk that was partially consumed, Oster connects the dots by first citing an old study finding that breastmilk is less susceptible to bacterial growth than formula, and putting that information together with the knowledge that partially drunk formula is safe up to 24 hours later. The preprint study comparably found that even 24 hours later, bacterial growth in partially drunk breastmilk was unconcerning.
Referencing mixing freshly pumped, warm milk into cold milk in the fridge, Oster writes, “we established above that, generally, breast milk is quite stable, and storage, even at room temperature, is safe for a fairly long time. Adding breast milk to a bottle—that is, slightly warming it for a brief period, while also leaving it in the refrigerator—is a very small change.”
We don’t know if breastmilk is safe longer than four days in the fridge
Oster observes that available research shows that up to four days in the fridge is safe for unused breastmilk [6]. This is the allowable limit according to the CDC guidelines, si the milk has not yet been reheated. Beyond day four, we just don’t have data yet, according to Oster. Future research needs to delineate the exact limit of breastmilk safety. The solution? Freeze the milk instead if you don’t anticipate using it within that four day limit.
Le bilan
With exemptions for babies born preterm, babies in the NICU, and babies receiving donor milk, Oster believes that for full-term, healthy babies, breastmilk storage guidelines could safely be relaxed to the following:
Before the bottle has been started, pumped breastmilk should be safe on the counter for up to 8 hours and in the fridge for up to 4 days.
Après the bottle has been started, pumped breastmilk should be safe on the counter for up to 8 hours and in the fridge for up to 24 hours.
While the CDC recommendations have not changed, Oster’s work provides some definite food for thought for those moms continually wondering if their milk is safe for their babies. Breastfeeding is often compared to a full-time job, requiring a great deal of time and energy for moms. And for the many moms who need to pump, the additional tasks of keeping equipment clean and milk properly handled and stored make the workload even greater. If Oster’s less-stringent recommendations were to be adopted, it would be welcome for many moms indeed.






